Find the revenue payers paid wrong
Alinea IQ reviews claims, remits, contracts, and payer behavior to identify underpayments, non-payments, and reimbursement patterns that are often missed in normal revenue cycle workflows.
We help providers turn payment variance into financial evidence for recovery, escalation, settlement, and contract protection.
Paid does not always mean paid correctly.
- Collaborative Evidence Workflow
- Contract Payment Intelligence
Paid claims can still hide major reimbursement loss.
Expected Payment Logic
Translate payer contracts, rate sheets, and fee schedules into expected reimbursement logic at the claim and line level.
Hidden Underpayment Detection
Identify paid claims that appear closed but were not paid according to contract, rate, or reimbursement expectations.
Payer Pattern Analytics
Group issues by payer, product, plan, service line, denial reason, variance, and root cause so teams can see whether a payment issue is isolated or systemic.
Who uses Alinea IQ
Finance Leaders
See where payer payment behavior is creating financial risk by comparing expected payment to actual payment across payers, products, contracts, and service lines.
Revenue Cycle Teams
Prioritize the payment issues that matter most, including paid claims, denied lines, non-payments, line-level variance, and repeat payer behavior patterns.
Managed Care and Contracting
Measure whether payer adjudication matches contract intent and turn payment variance into evidence for payer meetings, negotiations, amendments, and settlement discussions.
Compliance and Operations
Give operations and compliance teams a clearer view of payer behavior, reimbursement variance, payment exceptions, and the evidence needed to support internal review or escalation.
Turn contract language into payment accountability.
Contract Risk Signals
Identify contract terms, payment behaviors, and reimbursement patterns most likely to create underpayment exposure.
Connect payer, product, plan, contract, and reimbursement logic so your team can identify the real source of payment variance.
Recurring Payment Issues
Expose repeatable underpayment, non-payment, bundling, COB, and policy-driven adjudication issues that persist across claims and contract periods.
Show how contract terms, reimbursement logic, payer policies, and adjudication rules shape the final payment outcome.
Prevent Repeat Variance
Move beyond retrospective recovery by detecting repeated payment issues before the same variance continues across more claims.
Turn findings into recovery priorities, payer escalation packages, settlement support, and contract protection strategies.
Start with the claims already on your books.
If you believe your organization is being underpaid, over-denied, or affected by inconsistent payer payment behavior, Alinea IQ can help quantify the exposure and identify the root cause.
How Alinea IQ helps
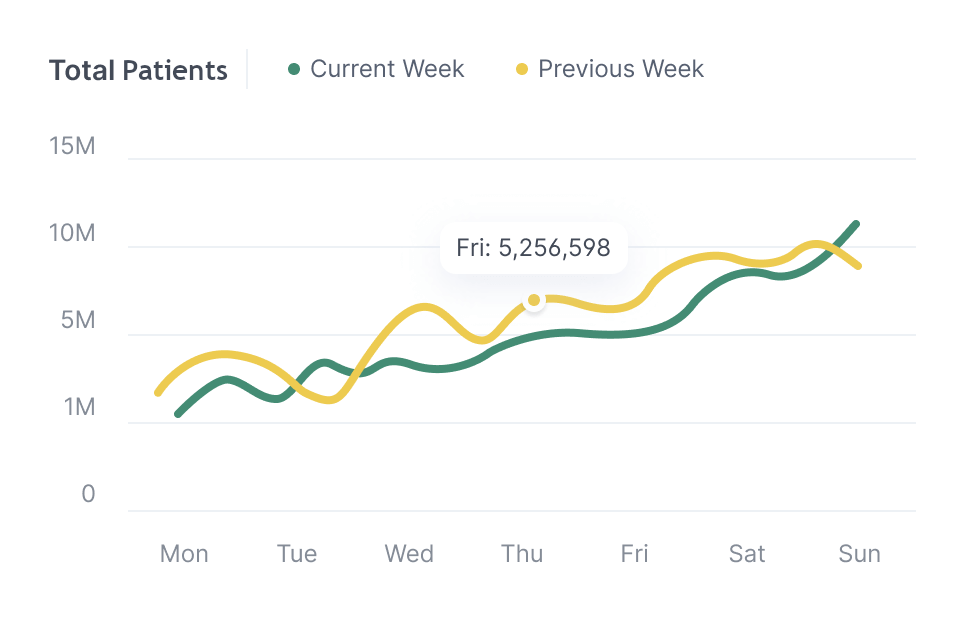

Find Hidden Payment Variance
- Identify underpayments, non-payments, and line-level variance
- Detect paid claims that were not paid correctly
- Quantify revenue already earned but not fully paid


Validate Contract Performance
- Compare actual payment to expected reimbursement
- Group issues by payer, product, plan, and root cause
- Show where adjudication does not match contract intent

Build Recovery and Contract Evidence
- Support payer engagement with claim-level and line-level evidence
- Prioritize issues for recovery, escalation, or settlement
- Use findings to improve future contract protection
Works With Your Existing
EHR and RCM Platforms
Alinea IQ works outside your production systems by analyzing exported claims, remits, contracts, rate sheets, and fee schedules without requiring a major EHR or billing system implementation.
Let's talk integrationSee where payers may be underpaying you.
Start with a focused payment review. Alinea IQ can help identify underpayment patterns, quantify exposure, and show which issues may require recovery, escalation, settlement, or contract protection.